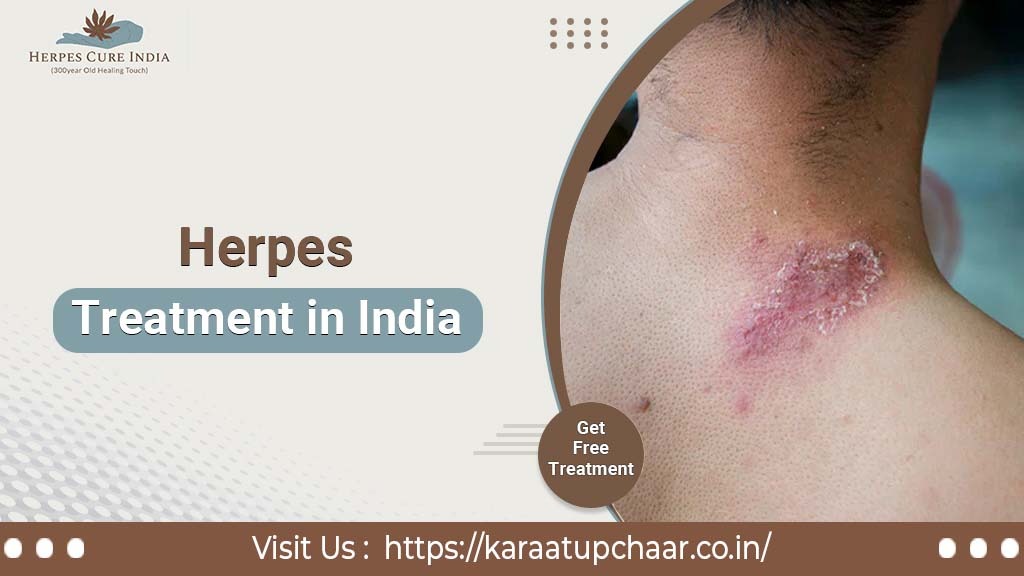
What is the Herpes Simplex Virus?
Herpes is a viral infection caused by the herpes simplex virus. HSV-1 and HSV-2 are two infectious diseases that cause this infection.
HSV1 (Herpes Simplex Virus-1)
HSV2 (Herpes Simplex Virus-2)
What is the Herpes Simplex Virus type 1 (HSV-1)
Herpes simplex virus type 1 (HSV-1) is a common virus that causes cold sores or fever blisters on the lips and mouth, as well as other types of infections. While there is no cure for HSV-1, there are several treatments available to manage symptoms and reduce the frequency and duration of outbreaks
Antiviral medications are often used to treat HSV-1 infections. Some commonly prescribed antiviral medications for HSV-1 include:
Genital infection is also adopted through sexually transmitted infection (STI). It even spreads via direct contact with the infected person’s body. Occasionally, the infected person sometimes does not even show any symptoms of the herpes simplex virus 1 but he or she can infect another person. A child can get infected during birth. The contagion, after infection, gets transported to the whim-whams cell bodies and it remains there idle lifelong.
What is the Herpes Simplex Virus type 2 (HSV-2)
Herpes simplex virus type 2 (HSV-2) is a common virus that is primarily transmitted through sexual contact. It can cause genital herpes, which is a sexually transmitted infection that causes painful sores or blisters on or around the genitals or rectum. While there is no cure for Herpes simplex Virus -2, there are several treatments available to manage symptoms and reduce the frequency and duration of Herpes outbreaks.
Genital infection is also adopted through sexually transmitted infection (STI). It even spreads via direct contact with the infected person’s body. Occasionally, the infected person sometimes does not even show any symptoms of herpes simplex virus 2, but he or she can infect another person. A child can get infected during birth. The contagion, after infection, gets transported to the whim-whams cell bodies and it remains there idle for lifelong
Some common antiviral medications for Herpes simplex virus -2 include:
Acyclovir (Zovirax)
Valacyclovir (Valtrex)
Famciclovir (Famvir)
These medications work by inhibiting the replication of the Herpes simplex virus 2, which can reduce the severity and duration of symptoms and help prevent future outbreaks.
What is the treatment medicine for Herpes simplex virus?
There are several medications available for the treatment of herpes simplex virus (HSV) infections. The specific medication prescribed will depend on the type and location of the infection (i.e., oral or genital), as well as the severity and frequency of outbreaks.
Antiviral medications are commonly used to treat Herpes simplex virus infections. These medications work by stopping the HSV virus from replicating and spreading to new cells. Some commonly prescribed antiviral medications for HSV infections include:
Acyclovir (Zovirax)
Valacyclovir (Valtrex)
Famciclovir (Famvir)
These medications can be taken orally or applied topically (on the skin) in the form of creams or ointments. They are most effective when started early in the course of an outbreak and taken for the full course of treatment as prescribed by a healthcare provider.
It’s important to note that while antiviral medications can help to manage symptoms and reduce the frequency and duration of outbreaks, they do not cure Herpes simplex virus infections. Additionally, these medications may not be appropriate for everyone and can have side effects, so it’s important to discuss any concerns or questions with a healthcare provider.
How to do Hsv-1 treatment?
HSV-1 (Herpes Simplex Virus 1) is a virus that can cause cold sores or fever blisters on the lips or around the mouth. but there are treatments available to help manage symptoms and reduce the frequency and severity of outbreaks.
Here are some options for HSV-1 treatment:
Antiviral medications: These medications can help to reduce the duration and severity of symptoms during an outbreak and can also be taken on a daily basis to help prevent future outbreaks. Examples of antiviral medications commonly used to treat HSV-1 include acyclovir, valacyclovir, and famciclovir.
Topical treatments: Over-the-counter creams and ointments containing numbing agents, such as lidocaine, can help to relieve pain and itching associated with cold sores. Applying a cold, damp cloth to the affected area can also help to soothe the skin.
Avoid getting hit: Outbreaks of herpes simplex virus-1 can be triggered by stress, fatigue, illness, or exposure to sunlight, among other factors. Avoiding these triggers can help to reduce the frequency of outbreaks.
It is important to note that while these HSV-1 treatments can be effective in managing symptoms, there is no cure for HSV-1. If you have symptoms of herpes simplex virus-1 or are concerned that you may have been exposed to the virus, it is important to speak with a healthcare provider for a proper diagnosis and HSV-1 treatment plan.
How to do Hsv-2 treatment?
Herpes simplex virus 2 (HSV-2) commonly causes recurrent infections affecting the skin, mouth, lips, eyes, and genitals. which is a sexually transmitted infection,
We have the best remedy oils for Herpes simplex virus 2 treatments, oils will help manage symptoms and reduce the frequency and severity of outbreaks and give quick relief in (HSV-2)
Common severe infections include encephalitis, meningitis, neonatal herpes, and disseminated infection. Mucocutaneous infections cause clusters of small painful vesicles on an erythematous base. laboratory confirmation by culture, polymerase chain reaction, direct immunofluorescence, or serologic testing can be done. Herpes simplex virus 2 Treatment is symptomatic; antiviral therapy with acyclovir, valacyclovir, or famciclovir is helpful for severe infections and, if begun early, for recurrent or primary infections.
Here are some options for HSV-2 treatment:
Antiviral medications: Antiviral medications can be taken to reduce the duration and severity of herpes simplex virus outbreaks, and may also be taken on a daily basis to reduce the frequency of outbreaks. Examples of antiviral medications commonly used for HSV-2 treatment include acyclovir, valacyclovir, and famciclovir.
Topical HSV-2 treatments: Topical creams and ointments, such as docosanol and lidocaine, can help to reduce pain and itching associated with genital herpes outbreaks.
Symptoms Of Herpes Simplex Virus
In numerous cases, there may not be any visible symptoms for this problem but they can still transmit the infection to other people who may have come in close contact. They remain asymptomatic for months and may appear completely after a time period of infection. Some of the common symptoms are pain during urination, pocks near the mouth and/ or genitals, greenishness, and itching. You may also witness flu-like symptoms like headaches, fever, fatigue, vaginal discharge, red pocks on the skin, blown lymph bumps, and dropped appetite.
Its symptoms most of the time appear around four days after exposure to the body. Herps are easily transmitted and spread forward in other organs of your body. It can lead to herpes keratitis, a condition of infection of the eyes and it causes eye discharge, pain, and a gritty feeling.
Some people have intermittent infections after the original herpes simplex virus infection and its symptoms include cold blisters near the mouth, ulceration or pocks on the cervix in women, burning sensation around the genitals, and red pocks. ultimately, the frequency of the infections becomes lower and the symptoms aren’t severe.
Causes of Herpes Simplex Virus
HSV-1 is mainly spread by oral contact and causes oral herpes (including cold sores), but can also cause genital herpes. HSV-2 is a sexually transmitted infection that causes genital herpes simplex virus.
Herpes Cure in India
There’s no treatment available to cure this viral infection. Croakers define specifics to get relief from the symptoms and to limit the spread of the infection. Antiviral medicines circumscribe the addition of contagion and reduce the symptoms. The symptoms can vanish without any drug but you need to consult your croaker for proper treatment. specifics like valacyclovir and famciclovir are given to cases to lower the chances of an outbreak and reduce the inflexibility of the symptoms.
For there’s no such herpes cure in India, thus you can also try some home remedies to treat the symptoms at ease at home with simple ingredients. Taking bath in interspersed water, abstaining from sexual conditioning, avoiding restrictive clothes, washing hands constantly, and taking painkillers will help you.
Why Is not There a Cure For Herpes?
Unlike other sexually transmitted conditions, like syphilis or gonorrhea, herpes is not caused by bacteria. Rather, herpes simplex virus is a contagion that penetrates specific cells in the body lying dormant for months or times between outbreaks.
In some people, the herpes contagion can develop in the body but remain asymptomatic, meaning they do not ever witness any outbreaks.
Because herpes simplex virus is a contagion, it’s not possible to “kill” a herpes infection completely like a bacterial infection. Cold sore treatments and ways to help fight the HSV- 1 and HSV- 2 contagions pullulate, however, which means herpes does not have to be a life-changing event.
Antiviral medicines can reduce the threat of spreading the contagion and help outbreaks, but the current drugs cannot fully cure the contagion in the way that antibiotics can kill bacteria. Antiviral specifics like valacyclovir are largely effective at treating both oral and genital herpes simplex virus, meaning people with herpes can live normal, problem-free lives.
What is Herpes simplex virus Treatment in India?
There is no cure for the genital herpes simplex virus. However, daily use of oil massage shortens herpes outbreaks.
How does the herpes simplex virus spread?
HSV-1 is mainly transmitted via contact with the virus in sores, saliva, or surfaces in or around the mouth. HSV1 can be transmitted to the genital area through oral-genital contact to cause genital herpes simplex virus.
What HSV-2 treatment is available for herpes?
There is no cure for herpessimplex virus. However, home remedies (daily use of oil massage) can prevent or shorten outbreaks.
What can I do, if I have herpes?
If you have been diagnosed with genital herpes simplex virus and need treatment for an outbreak. Then go to home remedies. Ramesh Ji from herpes cure treats herpes simplex virus free of cost. With this treatment, you get relief overnight. If you want to free treatment for herpes, then visit herpescure.in the website.
If you want to get free herpes treatment from us, then visit our website-
Call Us –
Trinagar Kamal Agarwal (Hargovind Chahcha) – 9013289821
FD 46, Pitampura Prachi Agarwal – 9811718621
Ramprastha, Vaisali, Noida Ravi Agarwal – 9911395464
Frequently Asked Questions (FAQ) About Herpes
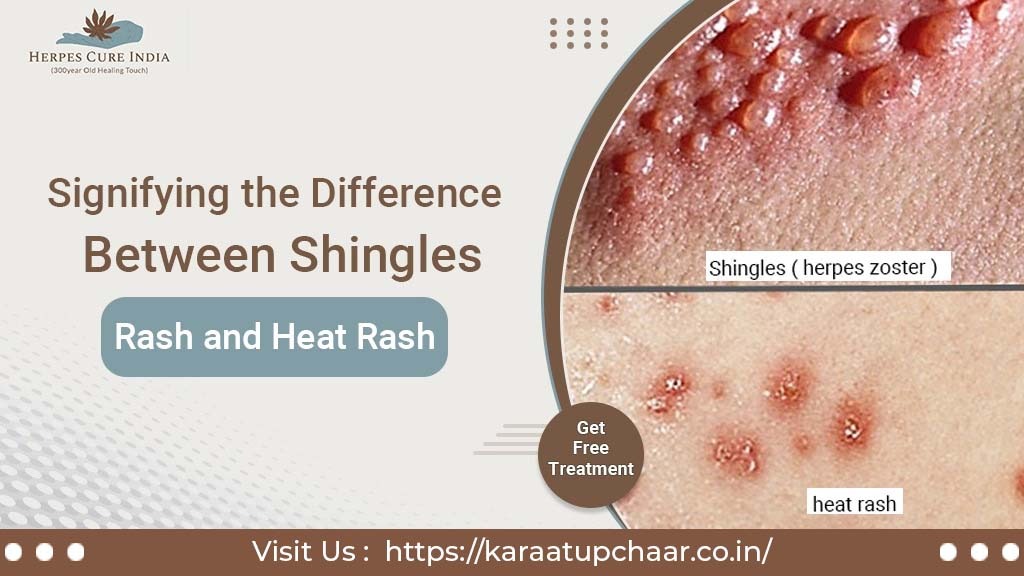
Yes, herpes can be painful. Both oral herpes (caused by HSV-1) and genital herpes (caused by HSV-2) typically result in painful sores and blisters. These lesions can cause significant discomfort, itching, and a burning sensation. During an outbreak, individuals may also experience flu-like symptoms, such as fever, body aches, and swollen lymph nodes. Herpes zoster (shingles), caused by the reactivation of the varicella-zoster virus, is particularly known for causing severe pain, often described as burning, throbbing, or stabbing. The pain can persist even after the rash has healed, a condition known as postherpetic neuralgia.
Can herpes cause nerve damage?
Yes, herpes can cause nerve damage, particularly in the case of herpes zoster, also known as shingles. Shingles can lead to a complication called postherpetic neuralgia (PHN), which occurs when the nerve fibers are damaged by the varicella-zoster virus. PHN is characterized by severe pain that can persist for months or even years after the shingles rash has healed. This pain results from the damaged nerves sending abnormal pain signals to the brain.
While less common, herpes simplex virus (HSV) infections can also cause nerve-related issues. For instance, HSV can lead to herpes simplex encephalitis, a rare but serious brain infection that can cause inflammation and damage to brain tissues and nerves. Proper medical treatment can help manage symptoms and reduce the risk of complications.