When Get Herpes Outbreak?
Herpes outbreaks can become at any time once a person is infected with the herpes simplex virus (HSV), which is a common sexually transmitted infection. The initial Herpes outbreak typically occurs within two weeks to a month of the initial infection, but sometimes herpes outbreaks may happen with varying frequency and severity. Outbreaks can be become by various factors such as stress, illness, fatigue, hormonal changes, and certain unused medications. It’s important to note that sometimes herpes can still be transmitted even when there are no visible symptoms, so practicing safe sex and disclosing your status to sexual partners is crucial in preventing its spread.
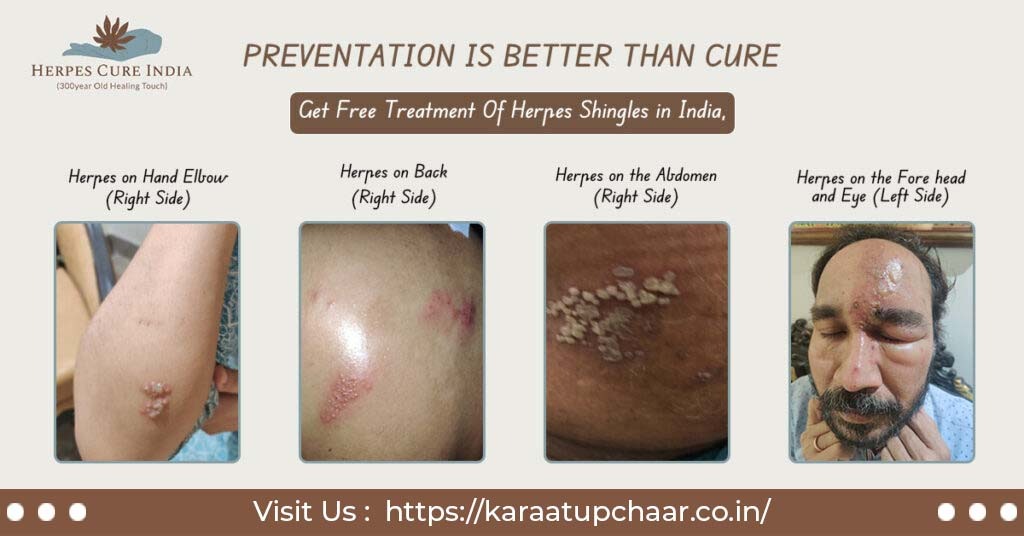
Use the following Points to protect from Herpes Outbreak
To protect yourself from a herpes outbreak, you can take the following steps:
1, Avoid close contact with someone who has an active herpes outbreak.
2, Do always have safe sex, including using condoms or dental dams during oral sex.
3, Avoid sharing personal items like towels, razors, or utensils with someone who has an active herpes outbreak.
4, Manage stress levels as high levels of stress can create herpes outbreaks.
5, Maintain a healthy lifestyle, including getting enough sleep, exercising regularly, and eating a balanced diet. Take antiviral medications as prescribed by a healthcare provider.
How do Stay Safe from Herpes Outbreaks During Pregnancy?
If you have genital herpes and are pregnant, it’s important to talk to your healthcare, and know how to reduce the risk of Genital (HSV) virus in Pregnancy’s women and her babies. Here are some tips to help stay safe from herpes outbreaks.
- Take antiviral medication: Your healthcare provider may prescribe antiviral medication to help prevent or reduce the severity of Herpes outbreaks during pregnancy.
- Do Practice Alway good hygiene: Wash your hands regularly and keep the genital area clean and dry to reduce the risk of infection for away herpes outbreak.
- Avoid sexual contact during outbreaks: If you or your partner has an active Herpes outbreak of herpes, avoid sexual contact until the outbreak has healed.
- Use condoms: Using condoms during sexual activity can help reduce the risk of transmitting herpes Outbreak to your partner or the baby.
- Consider a C-section: If you have active herpes lesions at the time of delivery, your healthcare provider may recommend a cesarean section to reduce the risk of transmitting the virus to your baby during delivery.
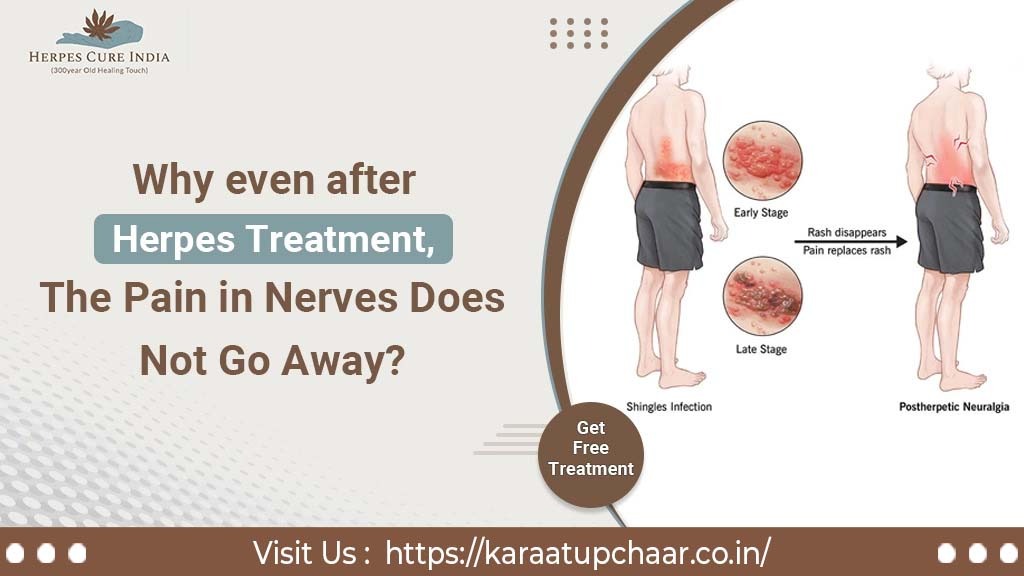
When herpes viruses come into contact with open sores or cuts on the skin, or when they enter the mouth, vagina, penis, or anus, they may spread. And the stages through which a person has to go are mentioned below:
Initial Herpes Outbreak Stage
Often, the initial outbreak of herpes is the most severe, and women typically have more severe symptoms than males. The initial outbreak normally occurs a few weeks after contracting the virus. The majority of symptoms often disappear within two to three weeks.
Multiple genital blisters are indicative of an initial (or main) bout of genital herpes outbreaks. According to gender, the most often afflicted areas are the vagina, vulva, buttocks, anus, and thighs for women, and the penis, scrotum, anus, buttocks, and thighs for males. Typical symptoms and indicators include blisters that progress into painful ulcers. On the penis or outer labia, blisters may harden and vanish. Up to five to seven days after the appearance of the first set of lesions, more lesions may emerge.
In addition, painful urination, sore, enlarged lymph nodes in the groin, and flu-like symptoms such as joint pain, fever, and headaches may be present. Some individuals may develop headaches, nausea, and vomiting, in addition to difficulty urinating. When the herpes outbreak simplex virus affects the nervous system, certain symptoms manifest. Proctitis (rectum or anus inflammation) can cause urination discomfort in some people. This problem is more prevalent among males who engage in sexual activity with others than among other patients.
Latent Stage: Following the first Herpes outbreak, the virus migrates to a clump of nerves near the base of the spine, where it finally stays dormant. This occurs during the latent stage. The stage has no symptoms.
Recurring episodes of the outbreak: Many people experience recurrent bouts of genital herpes, which occurs when the virus travels to the skin’s surface through nerves and causes an ulcer flare-up. The initial herpes outbreak was often much worse than these repeating episodes.
Ulcers may develop at new sites or return to the site of the original outbreak. Lesions may occur in areas where there was no direct touch, such as the anus region, where there was no anal intercourse.
The possibility of a herpes outbreak: many people with genital herpes, particularly those infected with HSV type 2, experience frequent relapses. Over time, recurrences often become milder and less frequent. A recurrence of the HSV infection a few years after the first infection is also possible. If you did not have symptoms after the first infection, this kind of delayed herpes outbreak may be distressing and cause you to worry about the behavior of your prior or present sexual partner (s).
Causes of Herpes outbreaks: illness, stress, sunlight, and tiredness can all cause herpes outbreaks to happen again and again. In women, an outbreak may be caused by their periods.
Note: Up to fifty percent of people who have a recurring outbreak have symptoms that occur before the formation of ulcers. This is referred to as the prodrome. Some instances of prodromal symptoms include itching, tingling, or discomfort in the buttocks, legs, or hips. Recurrences have a tendency to become less common and less severe once the first year has passed.
If you want to get free herpes treatment from us, then visit our website-
Call Us –
- Trinagar Kamal Agarwal (Hargovind Chahcha) – 9013289821
- FD 46, Pitampura Prachi Agarwal – 9811718621
- Ramprastha, Vaisali, Noida Ravi Agarwal – 9911395464
Frequently Asked Questions (FAQ) About Herpes
Can herpes spread?
Yes, herpes can spread from person to person through direct contact with an infected area. The two main types, herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2), are spread through different means. HSV-1, which commonly causes oral herpes, is typically spread through kissing or sharing personal items like utensils or lip balm. HSV-2, which primarily causes genital herpes, spreads through sexual contact. Both types can spread even when symptoms are not present due to asymptomatic shedding of the virus. Preventive measures include using condoms, taking antiviral medications, and avoiding contact during outbreaks.
Can herpes spread through air?
Herpes cannot spread through the air. The herpes simplex virus (HSV) requires direct skin-to-skin contact for transmission. HSV-1, responsible for oral herpes, spreads primarily through activities such as kissing or sharing utensils and personal items. HSV-2, which causes genital herpes, spreads mainly through sexual contact. Both types of herpes are transmitted via direct contact with infected sores, skin, or mucous membranes. The virus does not survive long outside the body, making airborne transmission or spread through casual contact highly unlikely. To prevent herpes transmission, avoid direct contact with sores and practice good hygiene.